Physical Well-Being Linked to Sharecare’s First Generation Social Determinant Index
Updated on July 27, 2020 at 2:30pm EST.
People’s physical health is closely tied to the conditions in which they are born, grow up, live and work, according to recent findings from Sharecare’s Community Well-Being Index (CWBI).
In January 2020, Sharecare launched its first-generation social determinants index (SDOH 1.0), which is founded in constructs tied to the federal government’s Healthy People 2020 framework. The index includes elements across ‘Neighborhood & Built Environment,’ ‘Health & Healthcare,’ ‘Social & Community Context’, ‘Education,’ and ‘Economic Stability.’
After examining the relationships between SDOH 1.0 and Sharecare’s Well-Being Index, which evaluates well-being across five different dimensions—physical, financial, social, community, and purpose—Sharecare and Boston University School of Public Health’s Biostatistics and Epidemiology Data Analytics Center found significant associations between rankings for physical well-being and social determinants of health.
The strong links underscore the importance of addressing health risks among individuals and within communities. This mission is fundamental to Sharecare’s community-driven approach to care, which focuses on deploying interventions across populations and regions that make healthy choices the easiest choices.
“Food insecurity is often the root of why individuals do not eat healthy, healthcare access is often the reason why individuals do not engage in critical preventative screenings that mitigate negative health outcomes, and the list goes on,” says Michael Rickles, PhD, Sharecare’s Executive Director of Research.
“In order to address health holistically, we must engage in a thoughtful approach that lends to understanding and addressing risk across multiple levels,” Rickles adds. “And that includes the social determinant risks that frequently define our ability to achieve a healthy life.”
The goal of the new index
By creating the SDOH 1.0, Sharecare sought to establish a first-generation social determinants of health view that aligned to the constructs well-known to the public health community through Healthy People 2020.
SDoH 1.0 mirrors and expands upon concepts established by the Centers for Disease Control and Prevention (CDC) as being salient for affecting the health of communities. The SDoH 1.0 Index and its component metrics are based on the CDC and the Department of Health and Human Services’ Healthy People 2020 categories but expand upon them in a meaningful way.
Sharecare utilized unique data points, drawn from peer-reviewed research, to create the composite measures. The final SDoH 1.0 index values were derived using exploratory factor analysis and other statistical techniques, which ensured that the metrics were valid and reliable.
“Leveraging variable reduction techniques and substantive expertise, Boston University’s Biostatistics and Epidemiology Data Analytics Center (BEDAC) translated more than 600 elements of social determinants of health data into 59 items that lend to initial visibility into how states, MSAs and counties rank when it comes to critical factors like greenspace, health insurance, and employment,” Rickles explains.
The conditions people encounter where they live, learn, work and grow have long been shown to affect their health risks and outcomes, according to the CDC. For example, higher education is linked to better health while poverty may prevent people from affording healthy foods and stable, safe housing. The CDC points out that the health and well-being of individuals and communities as a whole may be improved and disparities may be reduced by taking these social determinants of health into account.
What the new index revealed
Among the states with the highest levels of social determinants in Sharecare’s SDOH 1.0 Index:
- 1. Hawaii
- 2. Massachusetts
- 3. Alaska
- 4. Utah
- 5. New Jersey
On the opposite end of the rankings, the states with the lowest levels tied to Sharecare’s SDOH 1.0 Index include:
- 46. Tennessee
- 47. West Virginia
- 48. Kentucky
- 49. Arkansas
- 50. Mississippi
While examining the relationship between the SDOH 1.0 Index and Sharecare’s Well-Being Index however, Sharecare and Boston University School of Public Health’s Biostatistics and Epidemiology Data Analytics Center found highly similar patterns among physical well-being.
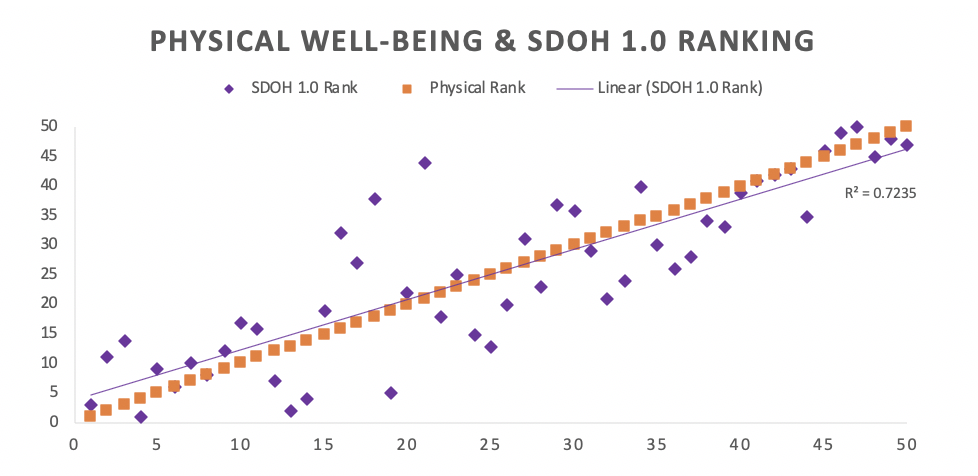
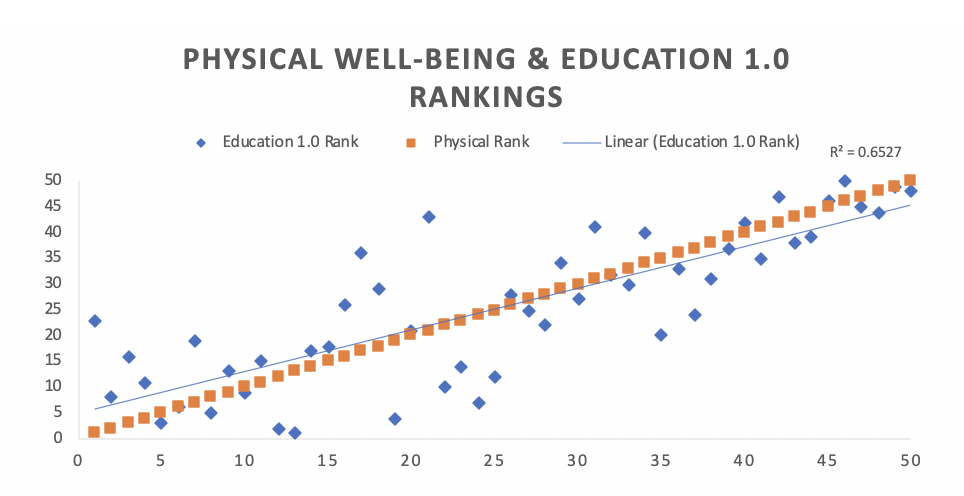
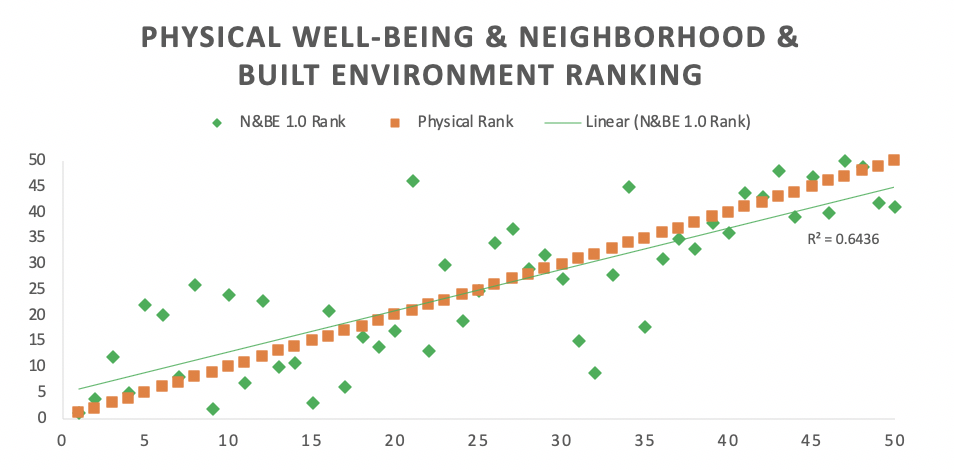
“Since relationships between social determinants and well-being have been proven out in other models, we were not surprised by the relationships,” Rickles says. “However, we were somewhat surprised about level of association between rankings.”
For the SDOH 1.0 measure overall, the majority of states who fell in the top 10 also fell in the top 10 rankings for the physical well-being element. Meanwhile, of the bottom 10 states for the SDOH 1.0 measure overall, 9 out of 10 states also fell in the bottom 10 states for physical well-being.
More specifically, SDOH 1.0 rankings across constructs, such as ‘Education’ and ‘Neighborhood & Built Environment,’ showed stronger associations with physical well-being rankings than other constructs, including economic stability and even health and healthcare.
“This is just the beginning of our journey to contextualize the relationships between individual and community health risk”, says Rickles, “with the largest longitudinal view of well-being nationally through the Sharecare Well-Being Index, we can bring these social determinants to life in a method and level of scale that has not been achieved previously.”
For additional information on SDOH 1.0 or Sharecare interventions targeted toward health improvement and outcomes, please reach out to CWBI@sharecare.com.