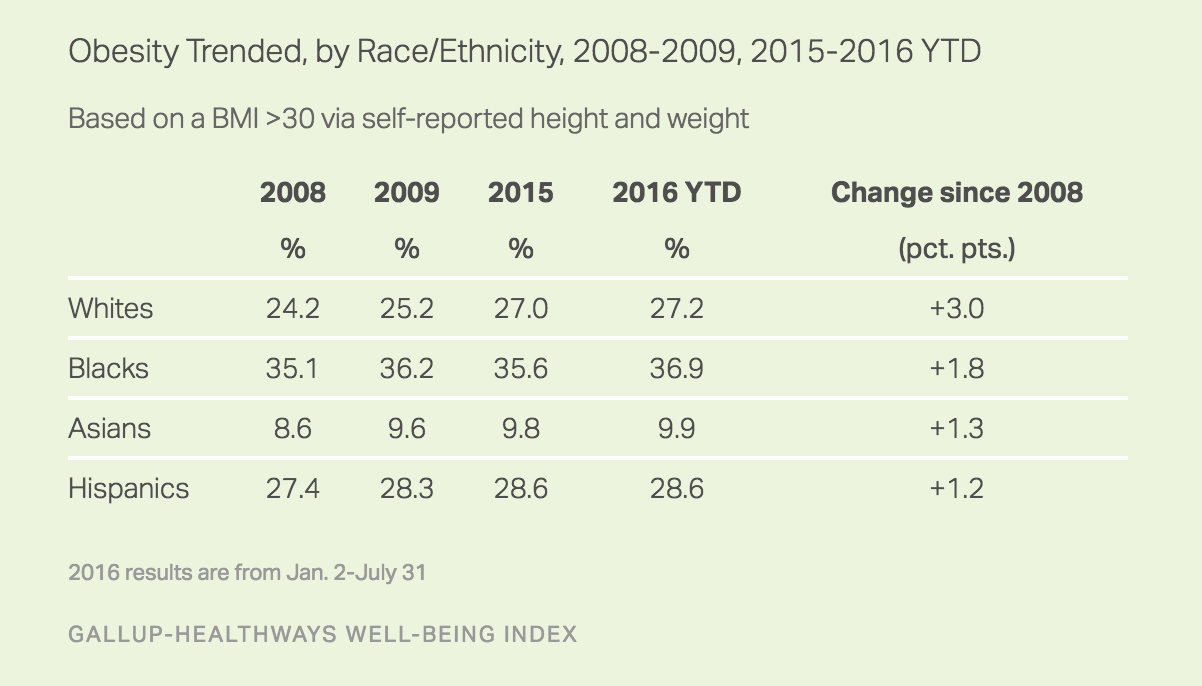Americans’ Health Assessments Worsen During Obama Years
STORY HIGHLIGHTS
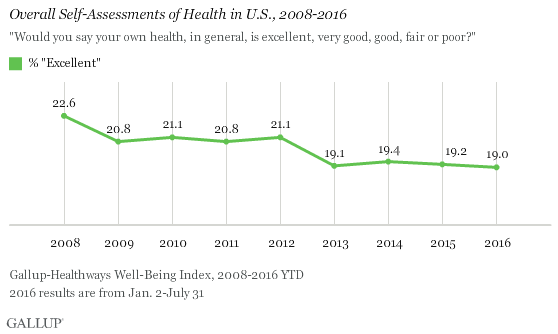
- Americans are less likely to report “excellent” health now than in 2008
- Obesity and diabetes rates are steadily climbing
- High cholesterol has declined across all major racial/ethnic groups
This is the fourth of a five-part series examining changes in Americans’ health and well-being during Barack Obama’s presidency.
WASHINGTON, D.C. — Americans’ self-assessments of overall health have slipped since 2008. Currently, 19.0% of U.S. adults report that their health is “excellent,” compared with 22.6% in 2008, before President Barack Obama took office. The percentage of U.S. adults who report “poor” or “fair” health has remained stable during this period at around 20%.
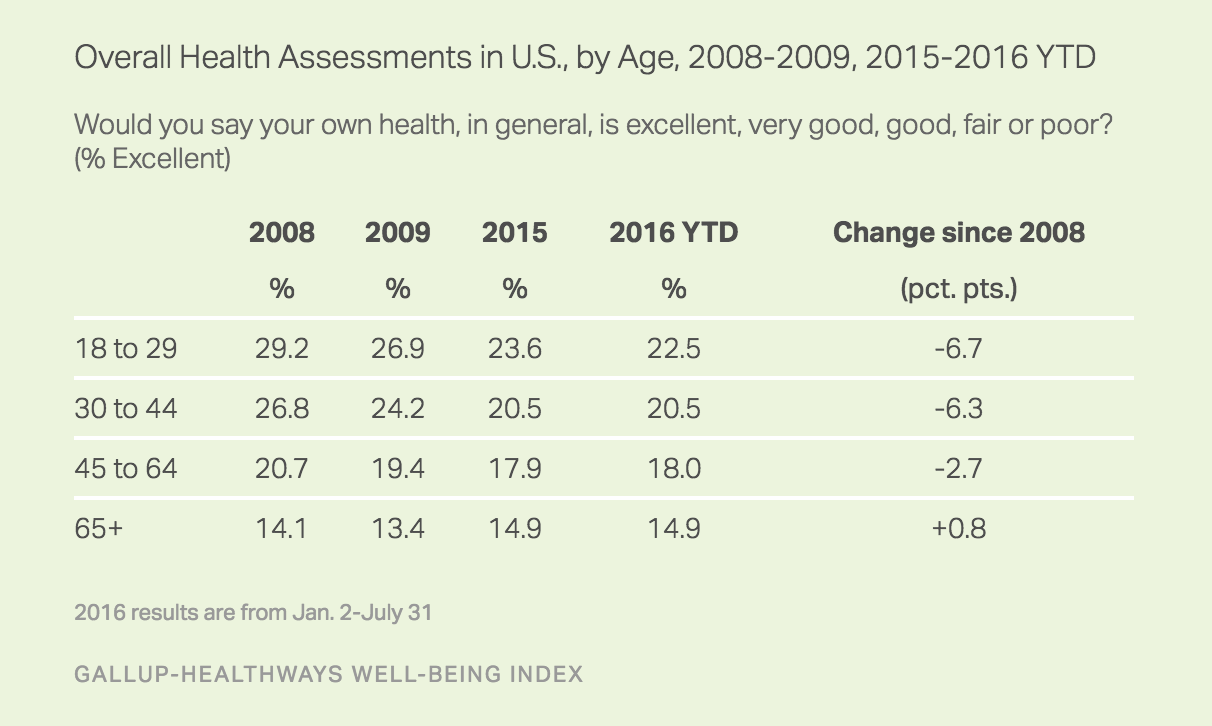
This drop in reports of excellent health since 2008 is largest among those younger than 45, with no change measured among seniors aged 65 and older. Personal health assessments worsened across all four major racial and ethnic groups — whites, blacks, Hispanics and Asians — with the greatest drops coming from Asians (down 5.5 percentage points) and whites (down 3.8 points). Blacks’ and Hispanics’ assessments each dropped by less than two points.
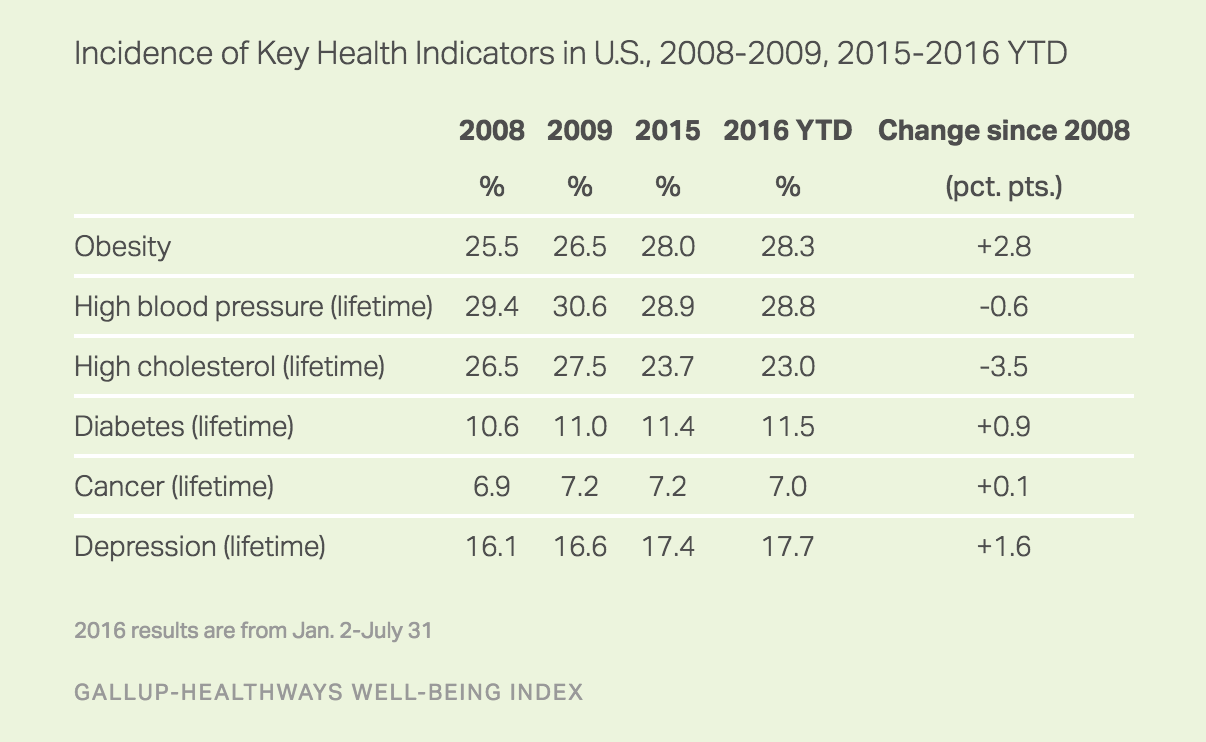
While the percentage of adults who consider their health to be excellent has declined, the percentage who report ever having been diagnosed with various major chronic diseases presents a more mixed picture. Since 2008, obesity has increased by nearly three points to 28.3%, and lifetime diagnoses of diabetes have increased about one point to 11.5%, a statistically significant climb. Self-reports of clinical diagnoses of depression have also edged up since 2008.
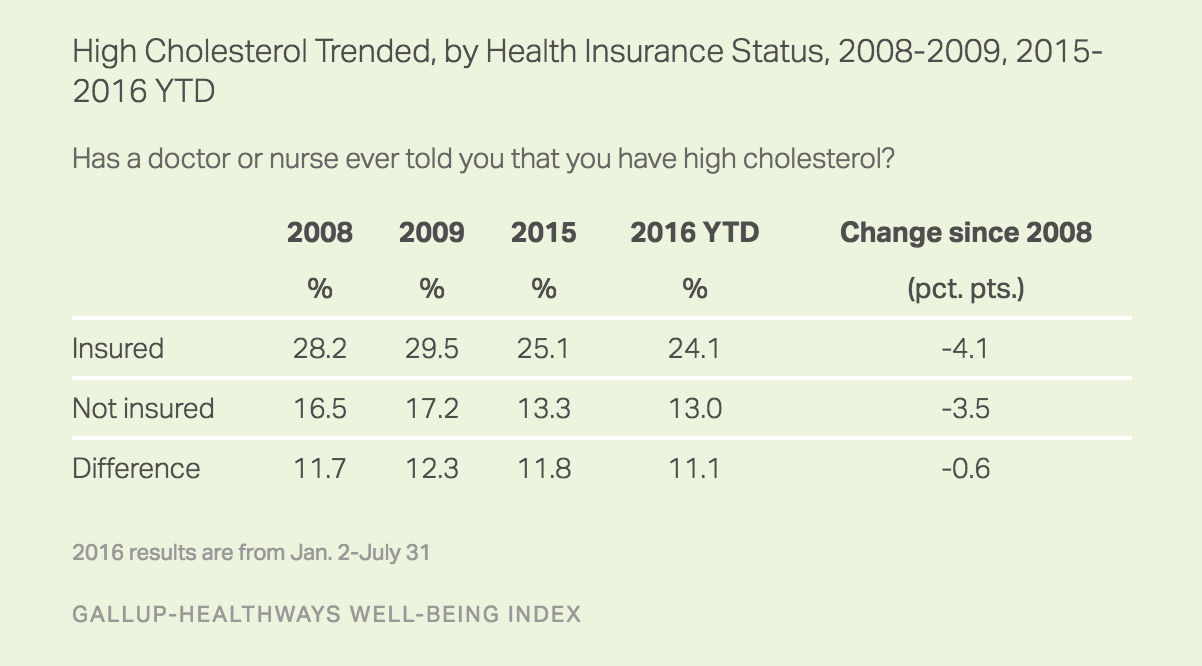
On the other hand, the percentage of Americans who report having been diagnosed with high cholesterol in their lifetimes has declined by 3.5 points since 2008, while reports of high blood pressure and cancer are essentially unchanged.
Historically, blacks have disproportionately suffered from chronic conditions, including obesity and high blood pressure.
These results are based on more than 100,000 interviews thus far in 2016, 175,000 interviews conducted in 2015 and more than 350,000 interviews conducted in 2008 and 2009 as part of the Gallup-Sharecare Well-Being Index. Unlike some government estimates of obesity, the Well-Being Index uses respondents’ self-reported height and weight to calculate body mass index (BMI). It does not involve in-home clinical measurements, which typically result in higher obesity rates at a population level. All other chronic conditions are measured based on responses to the question: “Has a doctor or nurse ever told you that you have ___?”
Obesity’s Overall Increase Driven Primarily by Whites
Whites’ obesity rates have risen more since 2008 than those of blacks, Asians and Hispanics. Overall, the obesity rate among whites has climbed three points to 27.2% thus far in 2016. The remaining three groups, in turn, have all seen their obesity rates increase by less than two points during that time.
High cholesterol is the one major chronic condition that has diminished in the U.S. adult population over the course of the Obama era, even as the rate of obesity, often associated with high cholesterol, has continued to climb. The percentage of adults who have been diagnosed with high cholesterol has decreased across all four major racial and ethnic groups in the U.S.
Those with health insurance are more likely to have been diagnosed with most of the aforementioned chronic diseases than are those without insurance. Declining uninsured rates since 2013 could theoretically be playing a role in the increasing percentage of adults who have been diagnosed with any given condition in 2016 compared with the pre-Affordable Care Act era in 2008 or 2009. A Gallup analysis demonstrates that this potential influence has at best only a minor effect on change in diagnosis rates, at least thus far.
Implications
Obama’s signature legislative achievement, the Patient Protection and Affordable Care Act (ACA), will ultimately be judged based largely on three major criteria: the reduction in the percentage of Americans without health insurance, the rate of increase in healthcare costs over time, and trends in the overall health of the American public. While the uninsured rate has declined since the ACA was fully implemented, the changes in various health conditions measured as a part of the Well-Being Index reveal a mixed picture.
The ongoing climb in both obesity and diabetes is likely tied to the decline in Americans’ overall self-assessments of their general health. The percentages of adults who have been diagnosed with high blood pressure and cancer, however, are essentially unchanged, while the proportion who report having been diagnosed with high cholesterol has noticeably declined. Smoking is linked to high cholesterol, so it is possible that the decline in the high cholesterol rate is related partly to the ongoing decline in smoking that began decades ago and has continued throughout the Obama era. Despite this positive trend, the rising obesity rate remains a significant problem, as its incidence in the population is closely linked to the other chronic conditions.
Obesity is most effectively addressed through both a holistic approach to well-being and a realistic and personalized plan. “A fundamental shift to lifestyle management is what we see on the horizon to help slow and reverse the rising rates of obesity in our country,” says Stacey Jensen, Senior Vice President at Sharecare. “It is not a one-size-fits-most approach, but rather one that provides precision planning around meals and exercise that is tailored to meet an individual’s needs. An effective plan should take into account topics such as what food individuals like, the amount of exercise they can commit to, and the availability of safe environments for exercise.”
While conventionally understood influences on obesity such as poor exercise, smoking and eating habits are all strongly linked to obesity, so too are less obvious factors such as not having a safe place to exercise, struggling to afford food, being from a low-income household and suffering poor social well-being. Therefore, taking a holistic approach that focuses on Americans’ purpose, social, financial and community well-being is an effective strategy to help reduce obesity and other chronic diseases, thus improving overall health in the U.S.
SURVEY METHODS
Results are based on telephone interviews conducted Jan. 2-Dec. 30, 2008-2015, and Jan. 2-Jul. 31, 2016, as part of the Gallup-Sharecare Well-Being Index, with a random sample of adults aged 18 and older, living in all 50 U.S. states and the District of Columbia. The national sample size was about 350,000 in 2008-2012, about 175,000 surveys in 2013-2015 and about 105,000 cases through the end of July 2016. In a typical year since 2013, about 130,000 whites, 16,000 blacks, 16,000 Hispanics and 4,000 Asians are interviewed. The margin of sampling error for each reported race or ethnic group is no more than ±1 percentage point in most cases, but climbs to ±1.6 percentage points for Asians in 2016. All reported margins of sampling error include computed design effects for weighting.
Each sample of national adults includes a minimum quota of 60% cellphone respondents and 40% landline respondents, with additional minimum quotas by time zone within region. Landline and cellular telephone numbers are selected using random-digit-dial methods.
Learn more about how the Gallup-Sharecare Well-Being Index works.